Introduction:
Globalisation and industrialisation have reshaped modern economies by driving technological progress, increasing productivity, and fuelling consumer demand. A crucial part of this transformation has been the creation and use of synthetic chemicals across industries and everyday products. While these chemicals have undoubtedly brought convenience and economic growth, they have also left behind an unintended legacy — widespread contamination of the environment due to improper handling, careless disposal, and weak regulation.
· In recent years, scientists have begun paying closer attention to a category of pollutants known as Contaminants of Emerging Concern (CECs). These substances are relatively new in terms of monitoring and regulation. They are not part of conventional water testing frameworks but are increasingly being detected in rivers, lakes, aquifers, soils, and even in treated drinking water. Because they remain largely unregulated and unmonitored, their potential impact on human health and ecosystems is a growing concern.
· Within this larger group of CECs, a particularly dangerous category has been identified — the Endocrine Disrupting Chemicals (EDCs). These chemicals are hazardous not only because they contaminate water and soil but because they interfere with the very system that governs biological growth, reproduction, and development: the hormonal or endocrine system.
Understanding Endocrine Disrupting Chemicals:
The World Health Organisation (WHO) defines endocrine disrupting chemicals as exogenous substances that mimic, block, or alter natural hormonal functions in the body, thereby producing harmful effects. Unlike many other pollutants that act only at high concentrations, EDCs can trigger disruption at extremely low levels, making them particularly insidious.
How EDCs Work:
EDCs interfere with the body in several ways:
· They may mimic natural hormones such as estrogen or testosterone and bind to receptors in cells, sending false signals.
· They can block hormones from binding to their receptors, preventing normal biological activity.
· They may disrupt hormone production, transport, or breakdown, creating long-lasting imbalances.
Health Impacts:
The consequences of such interference are wide-ranging:
· Developmental problems: affecting growth in infants and children.
· Reproductive disorders: infertility, reduced sperm quality, and altered sexual development.
· Neurological effects: learning disabilities, behavioural changes.
· Immune and metabolic issues: compromised immunity, obesity, diabetes.
· Transgenerational effects: impacts can be passed on to future generations.
Examples of EDCs:
Well-known chemicals in this group include:
· Bisphenol A (BPA): used in plastics and packaging.
· Phthalates: plasticisers found in many consumer goods.
· DDT and other pesticides: persistent pollutants that linger in soil and water.
· PFAS (Per- and Polyfluoroalkyl Substances): highly stable industrial compounds often referred to as “forever chemicals.”
· Synthetic hormones: such as estrogens used in contraceptives and medical treatments.
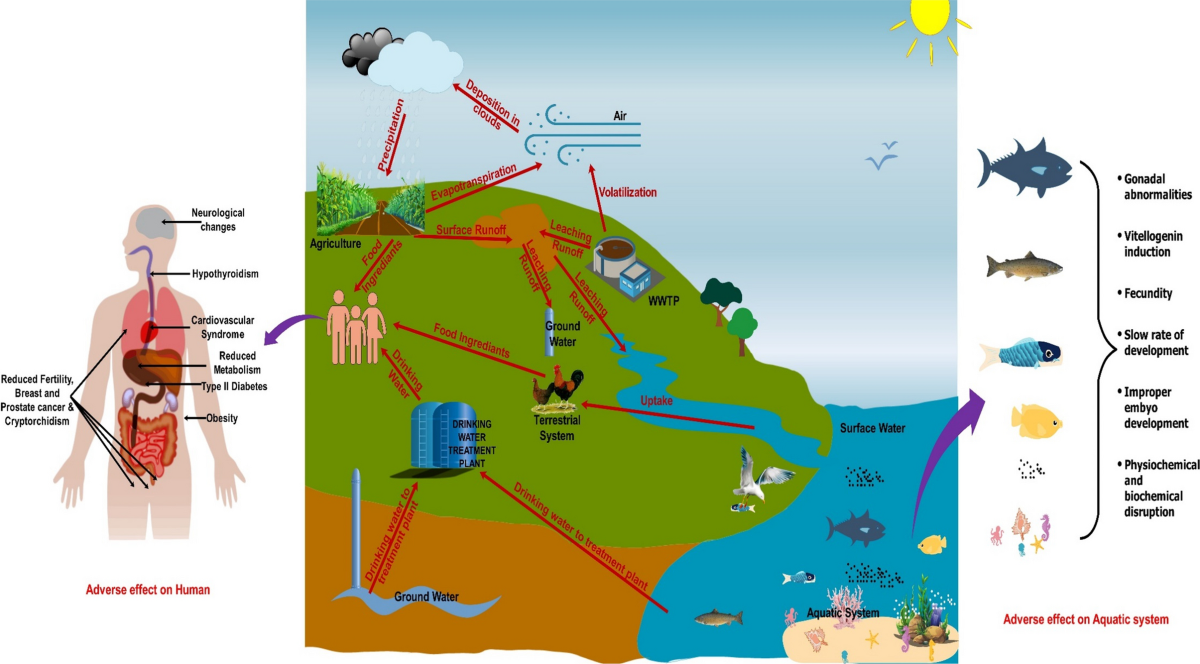
Pathways of EDC Entry into Water Systems:
EDCs enter India’s water systems through multiple overlapping routes:
1. Municipal Wastewater
o Natural hormones in human excreta.
o Residues of birth-control pills and other pharmaceuticals.
o Household chemicals and personal care products.
o Wastewater treatment plants are generally not designed to remove such micropollutants.
2. Agricultural Pesticides
o Extensive pesticide use contaminates rural aquifers and streams.
o Legacy pesticides like DDT, aldrin, heptachlor, and endosulfan can remain in soil for decades, slowly leaching into groundwater.
3. Pipes and Containers
o Water distribution systems and storage containers can themselves release BPA, phthalates, and metals such as antimony.
4. Pharmaceutical and Hospital Waste
o Effluents from pharmaceutical factories and hospitals may contain synthetic hormones (e.g., progesterone, estradiol) and antibiotics.
o Poor or absent treatment leads to direct release of these potent bioactive compounds.
Regulatory Gaps in India:
India’s regulatory framework is still silent on most EDCs. · BIS IS 10500:2012 (national drinking water standard) and CPCB norms prescribe limits for only a few older pollutants like DDT, aldrin, HCH, and PCBs. · Crucially, no standards exist for phthalates, BPA, PFAS, or pharmaceutical hormones. · There is no mandatory requirement to monitor drinking water or groundwater for these emerging contaminants. |
Global Contrast:
· The European Union’s Drinking Water Directive (2020) directly targets endocrine disruptors.
· A watch list mechanism requires EU states to monitor specific EDCs such as beta-estradiol and nonylphenol as an early warning system.
Indian Scenario:
· Very few long-term or national-scale studies exist.
· Academic findings often face denial from authorities. For instance, when researchers flagged PFAS in Chennai’s water, officials dismissed the claims citing their own limited tests.
· This highlights the need for systematic and transparent monitoring frameworks.
Strategies for Addressing EDCs in India:
1. Strengthening Regulations
o Revise BIS and CPCB standards to include safe limits for key EDCs.
o Expand monitoring to cover phthalates, BPA, PFAS, and pharmaceutical hormones.
2. Enhancing Monitoring and Laboratory Capacity
o Equip state and city laboratories with advanced instruments like Gas Chromatography-Mass Spectrometry (GC-MS) and Liquid Chromatography-Mass Spectrometry (LC-MS).
o Conduct nationwide, annual water quality surveys with open public data.
3. Improving Treatment Technologies
o Retrofitting large water treatment plants with advanced methods such as:
§ Activated carbon adsorption.
§ Ozonation.
§ Advanced oxidation processes (AOP).
§ Ultrafiltration and reverse osmosis membranes.
o These methods are internationally proven to reduce organic micropollutants and PFAS.
4. Decentralised and Nature-Based Solutions
o Constructed wetlands that allow reeds and microbes to naturally digest hormones.
o Small bioreactors for hospitals and industrial estates to neutralise phthalates and hormones before discharge.
o Low-cost, visible, and community-friendly systems suited to India’s needs.
Conclusion:
India’s water contamination challenge has entered a new and complex stage with the rise of endocrine disrupting chemicals. Unlike traditional pollutants, these chemicals act at trace levels, survive conventional treatment, and cause health impacts that may last across generations.
| Main question: Endocrine Disrupting Chemicals (EDCs) are emerging as a serious threat in India’s water systems. Identify two main pathways through which EDCs enter the water supply. Suggest two practical policy interventions to reduce such contamination. |